Background
From January 1 to April 26, 2019, 704 confirmed cases of measles have been reported in 22
states. This is the greatest number of cases reported in the U.S. since 1994 and since
measles was declared eliminated in 2000. These cases occurred primarily among
unvaccinated communities and are linked to travelers exposed to measles in countries with
ongoing outbreaks, such as Israel, Ukraine, and the Philippines. Since January 1, 2019, one
measles case has been reported in Missouri.
Given that ongoing measles transmission has not been identified in Missouri, the MMR
vaccine schedule recommendations have not changed at this time. There is no
recommendation from the Centers for Disease Control and Prevention (CDC) for
vaccination campaigns among adults or individuals in non-affected areas to prevent measles
outbreaks. One dose of measles, mumps, rubella (MMR) vaccine, or other presumptive
immunity, is sufficient for most U.S. adults born on or after 1957.
Measles Epidemiology
Measles is one of the most contagious of all infectious diseases; approximately 9 out of 10
susceptible persons with close contact to a measles patient will develop measles. The virus
is transmitted by direct contact with infectious droplets or by airborne spread when an
infected person breathes, coughs, or sneezes. Measles virus can remain infectious in the air
for up to two hours after an infected person leaves an area. Patients are considered to be
contagious from 4 days before until 4 days after the rash appears.
Healthcare providers should maintain a high index of suspicion for measles among febrile
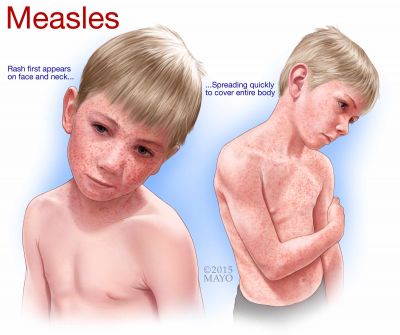
patients with a rash consistent with measles. A typical measles rash appears on the forehead
or the back of the head, then spreads downward to the trunk and extremities over the next
three days. Patients of all ages with clinical signs/symptoms compatible with measles
(febrile rash plus cough, coryza, and/or conjunctivitis) should be asked about recent travel
and contact with returning travelers, or contact with someone with a febrile rash illness. It is
also important to verify the patient’s vaccination status. Individuals who have been
previously exposed to measles antigen may have a modified disease presentation. All
persons exposed to measles regardless of vaccination status should monitor for symptoms of
measles for the 21 days after the last exposure.
Measles Prevention
Persons who have been exposed to measles should contact their health care provider if they
develop cold-like symptoms with a fever and/or rash consistent with measles. They should
NOT go to any health care facility without calling first. Health care facilities referring a
patient should also contact the receiving facility in advance of the patient’s arrival to avoid
additional exposures. The suspect case should be kept separated from others to prevent
further spread. Isolate suspect measles case-patients and immediately report suspected cases
to the local public health agency, or to DHSS at 573-751-6113 or 800-392-0272 (24/7). To
ensure prompt public health response, do not wait for laboratory confirmation.
The best way to stop the spread of measles is to be vaccinated. Two doses of MMR vaccine provides 97%
protection against the disease. One dose provides 93% protection.
The current general recommendations for MMR vaccination in areas not affected by measles outbreaks are:
For more detailed recommendations and contraindications for MMR vaccination, please see the References
section.
Measles Testing
The Missouri State Public Health Laboratory (MSPHL) provides laboratory support for the diagnosis of
measles infections occurring in Missouri. The MSPHL will only test specimens that are approved by state
public health officials. For questions regarding storage and shipping of all samples, please contact the MSPHL
Virology Unit at 573-751-3334.
Healthcare providers should obtain both a serum sample for IgM serology and a throat swab, nasopharyngeal
swab, or urine sample for RT-PCR molecular detection. Molecular samples should be collected along with
serum from patients suspected of having measles at first contact with them. See instructions for collection in
the References section.
Detection of measles RNA and measles virus isolation are most successful when samples are collected on the
first day of rash through the 3 days following onset of rash. Some patient samples may have detectable virus
up to 10 days post-rash onset. A negative RT-PCR result does not rule out measles because the test can be
affected by the timing of specimen collection and the quality and handling of the clinical specimens.
If the acute-phase serum sample is collected ≤ 3 days after rash onset and is negative, and the case
has a negative (or not done) result for RT-PCR, a second serum sample collected 3-10 days after
symptom onset is recommended because in some cases the IgM response is not detectable until 3
days after symptom onset.
Questions should be directed to DHSS’ Bureau of Communicable Disease Control and Prevention at 573-751-
6113 or 800-392-0272 (24/7).